IVF vs IUI: Differences, Success Rates, the Role of ICSI, and What You Really Need to Know
A Complete Guide to Understanding Fertility Treatment Pathways
When couples finally achieve pregnancy after months or even years of trying, often with the help of fertility treatments, an important question arises:
Is pregnancy achieved through IVF the same as pregnancy achieved through IUI, or does it require a different level of care from the very beginning?
The scientific answer is nuanced. While both methods can lead to the same outcome—a successful pregnancy—their medical pathways, level of intervention, reliance on medications, patient selection, and success rates are not the same.
As a result, care strategies are also different. A one-size-fits-all approach does not apply.

For some patients, IUI is a logical, less invasive option. For others, IVF is more effective from the start. And in certain cases, even conventional IVF is not sufficient, requiring ICSI (Intracytoplasmic Sperm Injection)—especially when male factor infertility plays a significant role.
This article goes beyond basic comparisons. We explore:
- Which method is suitable for which conditions
- Real-world success rates
- When ICSI becomes necessary
- How sperm quality (count, motility, morphology) changes treatment strategy
Because this is where awareness truly prevents confusion.
What Is the Fundamental Difference Between IVF and IUI?
IUI (Intrauterine Insemination) involves placing prepared sperm directly into the uterus at the optimal time. Fertilization still occurs naturally inside the body.
This means:
- Ovulation must occur naturally or be induced
- Sperm must reach the egg
- Fertilization and early embryo development happen
For this reason, IUI is closer to natural conception and is considered less invasive.
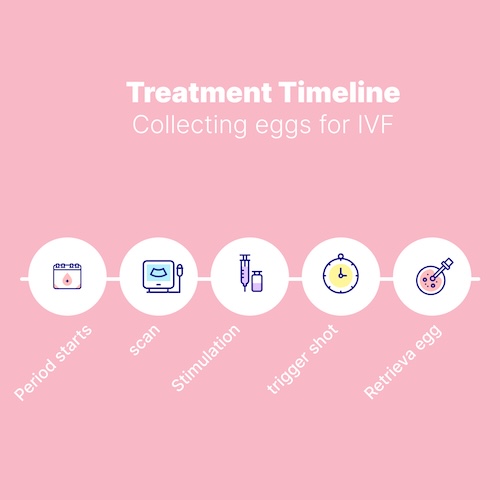
In contrast, IVF (In Vitro Fertilization) involves fertilization outside the body:
- Eggs are retrieved after ovarian stimulation
- Fertilization occurs in the laboratory
- One or more embryos are transferred into the uterus
This gives physicians greater control over fertilization and embryo development, making IVF more suitable for complex infertility cases.
Is IVF Always More Effective Than IUI?
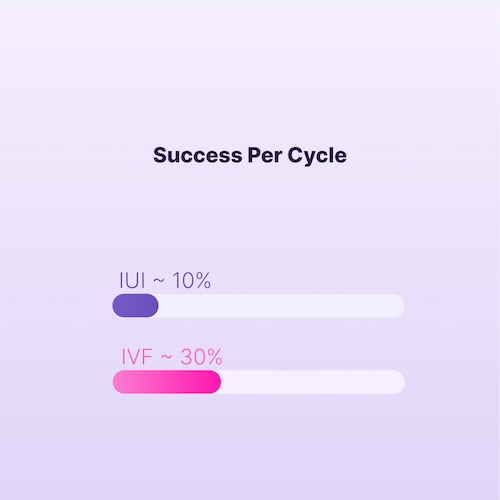
Generally, IVF has higher success rates per cycle, but this does not mean it should always be the first choice.
- IUI → simpler, cheaper, less invasive, lower success per cycle
- IVF → more complex, higher success per cycle
According to ASRM:
- Clomiphene + IUI → ~7.6% per cycle
- Gonadotropins + IUI → ~9.8%
- IVF → ~30.7%
However, NICE reports:
- Over 50% of women under 40 conceive after 6 IUI cycles
- Cumulative success may exceed 75%
👉 This shows an important point:
IUI should not be judged only by per-cycle success—it has cumulative value.
IVF Success Rates
According to HFEA (UK, 2023):
- Pregnancy rate per embryo transfer: ~31%
- Live birth rate: ~25%
- Age 18–34 → up to 41% pregnancy rate
- Success declines significantly after age 40
CDC data shows:
- ~37.5% of ART cycles lead to live birth
👉 The most critical factor remains:
IUI Success Rates
IUI success is lower per cycle:
- ~7–10% per cycle (ASRM)
- ~10% in women aged 35–40
- <5% in women over 40
However:
- Less invasive
- Lower cost
- Still effective in selected patients
The Role of Age in Choosing Between IUI and IVF
Age directly affects:
- Egg quality
- Chromosomal abnormalities
- Ovarian reserve
- Treatment success
👉 A woman at 32 may try multiple IUI cycles
👉 At 40, IVF is often recommended earlier
This is about time preservation, not just treatment choice.
What Is ICSI and When Is It Needed?
ICSI is a subtype of IVF.
Instead of natural fertilization in the lab:
👉 A single sperm is injected directly into the egg
HFEA recommends ICSI when:
- Very low sperm count
- Poor motility
- Abnormal morphology
- Previous IVF fertilization failure
However, ASRM states:
👉 In non-male factor infertility, ICSI does NOT necessarily improve live birth rates
When Does Sperm Quality Change the Treatment Strategy?
Severe sperm issues can shift treatment decisions:
- Very low count
- Poor motility
- Abnormal morphology
- Azoospermia
According to AUA/ASRM (2024):
- Genetic testing (Y chromosome microdeletion) may be needed
WHO (2021) also emphasizes standardized semen evaluation.
👉 Treatment decisions must be based on accurate interpretation, not a single test result.
Is IVF Always the Better Choice?
Not necessarily.
IUI is often preferred when:
- Mild infertility
- Open fallopian tubes
- Ovulation is present
- No severe male factor
IVF is preferred when:
- Advanced age
- Time is critical
- Multiple failed IUIs
- Complex infertility
Practical Summary
- Mild cases → IUI
- Time-sensitive or complex → IVF
- Severe male factor → IVF + ICSI
Final Conclusion
IVF and IUI lead to the same goal—but through very different paths.
- IUI → simpler, less invasive, lower success per cycle
- IVF → more complex, higher success per cycle
- ICSI → targeted solution for fertilization issues
👉 The key message:
Choosing between IUI, IVF, and ICSI is not choosing between treatments—
it is choosing between different treatment strategies.